
The expression
“sacred cow” is defined as an idea, custom, or institution considered
exempt from criticism. If you study the history of medicine or science,
you will find many ardently embraced sacred cows that eventually
staggered and collapsed.
Past is
prologue. This is not just a reflection of an unenlightened past, in
which, for example, authorities persecuted Galileo for advocating
heliocentricity or the 19th-century physician Ignaz
Semmelweis for audaciously recommending hand washing for surgeons, but
very much a contemporary issue. As a former scientific director of a
half-billion dollar institute at the National Institutes of Health, I
know first-hand that sacred cows still shape our health and nutritional
policy.
Influenced by
profit-making agendas, one modern-day sacred cow is the belief we need
to lower cholesterol levels at all costs through either taking
side-effect-laden drugs or eating foods that humans never
physiologically evolved to consume in quantity (e.g., trans-fats).
Natural-foods advocate and author Sally Fallon called high cholesterol
“an invented disease, a problem that emerged when health professionals
learned how to measure cholesterol levels…” According to George Mann,
former Vanderbilt University Professor, the cholesterol " myth is the
greatest scientific deception of this century, perhaps of any century."
As cited in
the resources, there are countless studies documenting 1) cholesterol’s
benefits, 2) health risks of having too low cholesterol, and 3)
eye-opening side effects associated with cholesterol-lowering drugs. The
evidence presented in such studies is often ignored, trivialized, or
statistically manipulated because it challenges prevailing health-care
policies - which like aircraft carriers take a long time to change
direction.
Cholesterol’s Role
In spite of
its vilification, cholesterol is an absolutely essential molecule,
especially for brain and spinal-cord functioning. Accumulating evidence
suggests that pushing down cholesterol levels through drugs over time
may have adverse neurological consequences. Given the molecule’s
paramount importance in the nervous system, some speculate that such
efforts may compromise neurological recovery after traumatic spinal-cord
or head injury.
Most of our
cholesterol comes not from food but is produced by the body, especially
the liver. Generally, our bodies synthesize three to five times more
cholesterol than we consume. Notwithstanding the indoctrination
otherwise, cholesterol levels are influenced very little by diet. For
example, the Maasai, an African nomadic tribe who traditionally ate more
animal fat than virtually any other population, had some of the world’s
lowest cholesterol levels. Although there may be other health
consequences, if we eat a large ham-and-cheese omelet for breakfast and
a bacon cheeseburger with a milkshake for lunch, our bodies just produce
less cholesterol. If we eat an ascetic vegetarian diet, our bodies will
produce more cholesterol.
In contrast,
by interfering with cholesterol biosynthesis, commonly prescribed statin
drugs (e.g., Lipitor), are extremely effective in lowering cholesterol.
However, they also compromise the production of several other substances
vital for health, including 1) coenzyme Q10 critical for energy
metabolism and heart and muscle health, and 2) dolichol, a fatty
molecule crucial in the assembly of cellular proteins.
Cholesterol is
an essential structural component of all cells, needed to ensure
membrane integrity, permeability, and fluidity. It has a key role in the
transport of molecules into the cell, interaction between cells, and,
importantly for PN readership, nerve conduction. The amount of
cholesterol in the CNS is about 10 times greater than any other organ.
If one is trying to rebuild a damaged nervous system, does it make sense
to take away the supply of essential building blocks through
cholesterol-lowering drugs?
In addition,
cholesterol is the precursor to a variety of sex hormones, including
testosterone, progesterone, and estrogen, and adrenal-gland hormones,
such as the stress hormone cortisol. Given that SCI already compromises
production of function-restoring testosterone (PN October 2011),
one can only speculate on the additional impact of pushing down the
levels of cholesterol, a testosterone precursor.
In addition,
the sun’s ultraviolet rays convert cholesterol in skin into vitamin D,
which is a vitally important nutrient for individuals with SCI and MS.
Finally, the liver uses cholesterol to produce bile, needed for fat
digestion in the small intestine.
Problems
with Low Cholesterol
Several
adverse health consequences connected to low cholesterol include:
Mental
Health: Low cholesterol is
associated with various mental-health issues. For example, research
suggests that individuals with too low cholesterol 1) have more
depression, 2) commit more suicide, 3) exhibit greater violent and
aggressive behaviors, 4) relapse more in cocaine addiction, 5) have
reduced attention, concentration, and word fluency, and 6) in the
elderly, have more cognitive decline and dementia. Lower cholesterol
levels lead to decreased brain levels of serotonin, a feel-good
neurotransmitter that Prozac-like drugs attempt to stimulate.
Infectious
Disease: Low cholesterol is
correlated with an increased risk of dying from various infectious
diseases. For example, in a study involving 100,000+ subjects,
individuals with lower cholesterol were admitted more often to a
hospital due to infectious disease.
Longevity:
Low cholesterol in the elderly increases risk of dying. A study
published in the prestigious journal Lancet concluded that in the
elderly “long term persistence of low cholesterol concentration actually
increases the risk of death.”
Heart
Disease: In spite of the hype
otherwise, many studies indicate little correlation between cholesterol
levels and heart disease. For example, although Americans have higher
cholesterol than Japanese, the arteries of Japanese people were just as
atherosclerotic – i.e., factors other than cholesterol must be involved.
Norwegian
Study
Given
editorial constraints, it’s difficult to summarize the numerous studies
whose results counter the cholesterol-lowering dogma. In one recent
example, researchers investigated the relationship between cholesterol
levels and mortality rates in over 52,000 Norwegians.
Although
cholesterol has been subdivided into “good” and “bad" cholesterol
depending upon its sequestering into greater complexes (e.g., high-
density and low-density lipoprotein), the investigators focused on
total cholesterol levels because health policies use this number to
determine treatment. Using official guidelines, 75% of Norwegian adults
are considered at risk for cardiovascular disease and, hence, “in need
of clinical attention.” About 47% of the subjects were men and 53%
women. Age ranged from 20-74. Subjects were followed for 10 years.
The
relationship of mortality to cholesterol levels were gender dependent.
For men, mortality followed a U-shaped pattern. Specifically, the
greatest mortality was observed in men with the lowest cholesterol
levels, the least mortality noted in men with intermediate cholesterol
levels, and in-between mortality documented in men with the highest
cholesterol levels.
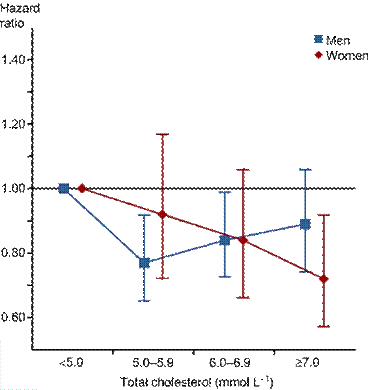
With women, it
followed a downward, linear pattern, in which cholesterol levels were
inversely related to death rates. Specifically, as levels increased, the
risk of death decreased; i.e., more cholesterol was associated with
living longer. In both men and women, the highest death rate was
associated with the lowest cholesterol levels.
The
investigators diplomatically concluded that given their results,
“clinical and public-health recommendations regarding the dangers of
cholesterol should be revised. This is especially true for women, for
whom moderately elevated cholesterol (by current standards) may prove to
be not only harmless but even beneficial.” Undiplomatically, it is yet
another stumble of a public-health sacred cow.
Conclusion
German
philosopher Arthur Schopenhauer stated “All
truth passes through three stages. First, it is ridiculed. Second, it is
violently opposed. Third, it is accepted as being self-evident.” The
notion that cholesterol needs to be lowered at all costs is so
passionately embraced by medical authorities that any suggestion
otherwise, regardless of merit, is virulently opposed. But it’s just a
matter of time before a more balanced viewpoint will prevail.
Part 2 will more closely look at the critical
role of cholesterol in the nervous system and review the multitude of
side effects, including neurological, associated with using
cholesterol-lowering drugs.
Adapted from article
appearing in June 2012 Paraplegia News (For subscriptions, call
602-224-0500) or go to
www.pn-magazine.com.
TOP